What Is Blood Cancer?
An introduction to blood cancers and blood disorders.
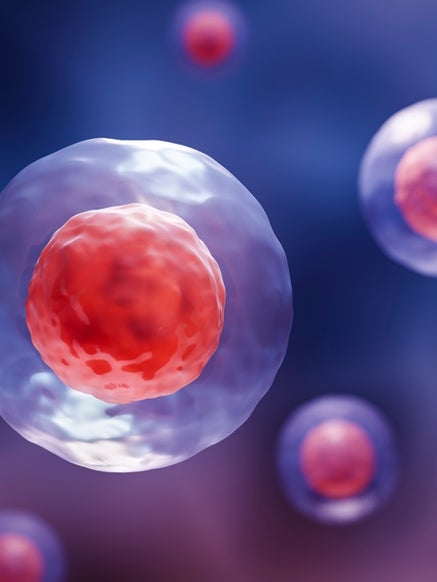
Blood cancers and blood disorders are caused by changes in the genes of blood cells or stem cells.
These changes affect the balance of cell growth and function within the body, particularly affecting the bone marrow — which is the soft centre of your bones where blood cells are born. This problem leads to the growth of abnormal blood cells that don’t do their job properly, like fighting infections, carrying oxygen, and helping wounds heal.
Blood cancers
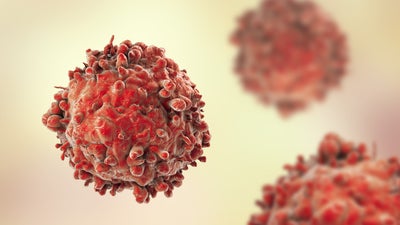
What is blood cancer? Blood is composed of plasma and blood cells. Plasma, the liquid part, carries cells, nutrients, and waste around the body. Blood cells include red cells that carry oxygen, white cells that fight infections, and platelets that help with clotting. Cancer of the blood typically involves the abnormal and excessive growth of white blood cells.
There are three main types of blood cancer. Leukaemia affects white blood cells and impairs the body's ability to fight off infections. It can develop in different forms: acute lymphoblastic leukaemia is more common in children, while chronic types are usually seen in older adults. Myeloma is a cancer of plasma cells, which are crucial for producing antibodies that help us fight off infections. This type of cancer makes the immune system weaker, increasing risk of illness. Lymphoma targets the lymphatic system, which is a part of the immune system and includes the lymph nodes, spleen, and thymus gland. It is broadly divided into Hodgkin lymphoma, identified by Reed-Sternberg cells, and non-Hodgkin lymphoma, which includes many different subtypes. This cancer impacts how the body produces and uses immune cells, leading to a higher risk of infections and other health issues.
Understanding blood cancer causes can be complex, as they are not always clear. In many cases, blood cancer develops due to genetic mutations in blood cells, sometimes influenced by factors such as age, environmental exposures or certain medical conditions
There are a number of common blood cancer symptoms, although they can vary depending on the type of blood cancer. These may include: unusual and persistent tiredness, unusual bleeding or bruising, severe night sweats, frequent infections, bone pain, and swollen lymph nodes.
Learn more: Types of blood cancer
Blood disorders
While blood cancers involve the malignant growth of blood cells, blood disorders are conditions that prevent your blood from functioning properly. These might include conditions that affect how your blood clots or how it stops bleeding. Blood disorders can impact any of the primary components of blood.
Blood disorders affect various components of your blood and have distinct impacts on health. Disorders such as anemia, polycythemia vera, and thalassemia impair the function of red blood cells, hindering the body's ability to carry oxygen where it's needed. White blood cell disorders, such as leukopenia and leukocytosis, affect the body's ability to fight off infections. Platelet disorders, including thrombocytopenia, thrombocythemia, hemophilia, and Von Willebrand disease, can lead to excessive bleeding or clotting issues. Additionally, plasma-related disorders involve the liquid component of blood, crucial in the clotting cascade, and influence both clot formation and bleeding, thereby maintaining a balance between these two critical functions.Top of Form
Some blood disorders are due to a specific gene fault inherited from your parents. If you’re born with a disease like sickle cell disease or thalassaemia, you will have inherited the gene fault from both parents to have the disease. Today, there is screening for these gene faults in some communities where they are more common.
There are also conditions that are a mix of a blood disorder and cancer. Myelodysplastic syndromes (MDS) are like this. They mean your bone marrow cells are not normal; they're a bit like cancer cells, but not quite. This is why people with MDS have a higher chance of getting leukemia because their cells already have some issues that are like cancer.
Learn more: Types of blood disorders
Living with blood cancer or blood disorder
Approximately 120,000 people living in the UK are affected by blood cancer, and every 14 minutes, someone is diagnosed. Thankfully, the outlook has significantly improved over the years, thanks to medical advancements. Treatments are continually evolving, offering hope and providing more people with second chances at life.
If you have been diagnosed, it can be empowering to learn more about your condition. Knowledge can help you make informed decisions about your treatment and care, and it can also help alleviate some of the fear and uncertainty that comes with a diagnosis of blood cancer or blood disorder.
The journey through blood cancer and blood disorders is unique for everyone, and there's no ‘right’ way to feel or cope. It's okay to seek help, and it's okay to lean on others. With the ongoing advancements in treatment, there is hope. Understanding your diagnosis might feel overwhelming, and your journey may be challenging, but there is an ongoing, global effort focused on improving the lives of patients with blood cancer and blood disorders.
This effort includes advancing research, improving treatments, and supporting those affected every step of the way. At DKMS, we have a database of 12,500,000 potential stem cell donors globally, and have facilitated over 125,000 donations from them over the years. We are fully committed to helping you, so please reach out to us to learn more or get involved.
Learn more: For patients and their loved ones
References
1. Blood cancer. Very Well Health. Accessed July 2024.
2. Blood disorders. Cleveland Clinic. Accessed July 2024.
3. Blood cancer fact sheets. Accessed July 2024.