Blood cancer: Myeloma
Overview
Myeloma is one of the three main types of blood cancers, alongside leukaemia and lymphomas.
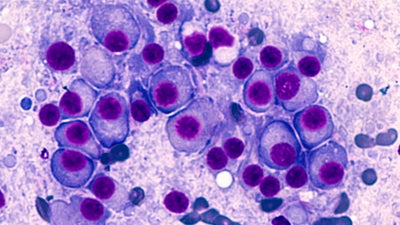
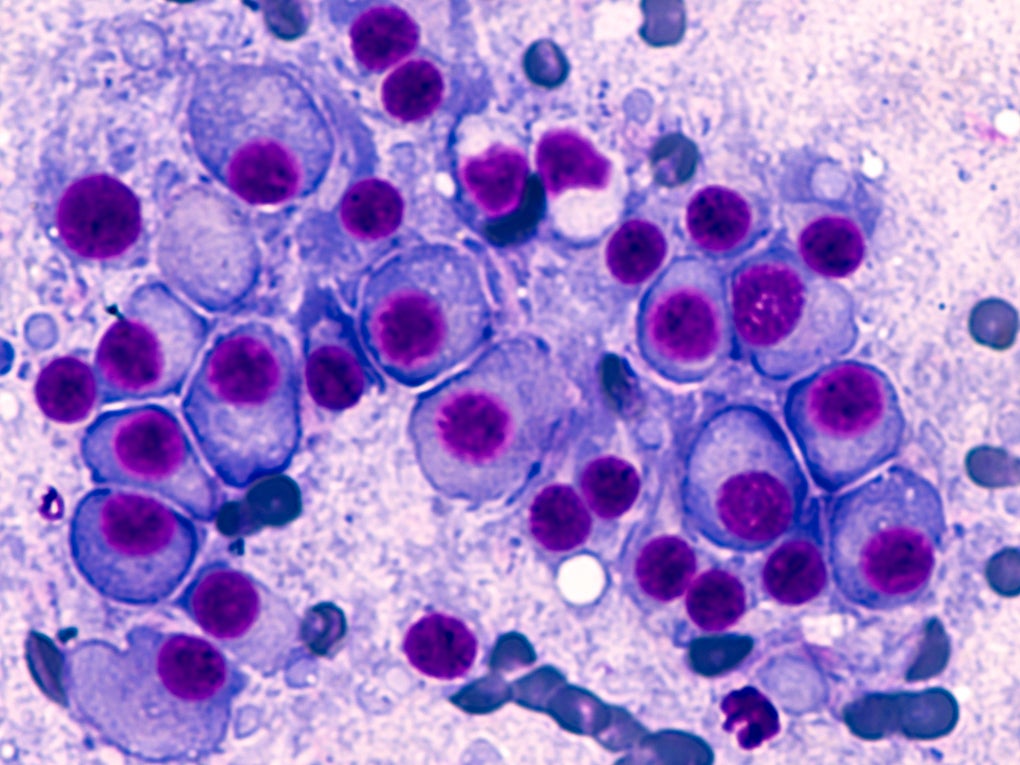
Myeloma, often referred to as multiple myeloma, is a type of blood cancer that primarily affects plasma cells in the bone marrow. Plasma cells are vital components of the immune system, responsible for producing antibodies that help fight infections.
In myeloma, these cells grow uncontrollably and produce abnormal antibodies known as paraproteins or monoclonal proteins. Unfortunately, these abnormal antibodies are unstable and cannot effectively fight infections.
If you or someone you care about has been diagnosed with myeloma, it's important to understand that this condition can vary greatly in how it affects each individual. While the cause of myeloma remains unclear, it is known to predominantly affect older adults, with a higher occurrence among men. Risk factors include a family history of the disease and certain ethnic backgrounds.
Additional factors such as obesity and exposure to certain chemicals or radiation may also increase the risk of developing myeloma. Understanding the risk factors, symptoms, and treatment options can empower you and your family as you navigate this challenging diagnosis together.
Learn more: Blood cancer
Recognizing Myeloma symptoms
Myeloma affects various parts of the body, and its symptoms can be grouped based on the areas they impact:
Bone-related symptoms
Pain: You may experience persistent or worsening pain, especially in your back. This discomfort is often due to the accumulation of cancerous plasma cells in the bone marrow.
Risk of fractures: The weakened bones in your arms, legs, shoulders, spine, skull, pelvis, and rib cage are more prone to fractures.
High calcium levels: When bones are damaged, calcium can leak into the bloodstream, leading to symptoms like extreme thirst, frequent urination, confusion, and drowsiness.
Kidney-related symptoms:
Renal impairment: The abnormal paraproteins produced by myeloma cells can harm your kidneys, potentially leading to kidney damage.
General health effects:
Fatigue: Anaemia, or a decrease in red blood cells, can leave you feeling extremely tired and weak.
Recurrent infections: Due to the ineffective abnormal antibodies, you might find it harder to recover from infections.
Loss of appetite and general sickness: Myeloma can affect your overall well-being, causing you to feel sick and lose your appetite.
Treatment options for Myeloma
Treating myeloma involves a mix of methods designed to target the disease and relieve symptoms:
Targeted treatments and chemotherapy: These drugs are designed to specifically target the cancerous plasma cells, reducing their numbers and helping to control the spread of the disease. This approach is vital in managing myeloma and preventing its progression.
Bisphosphonate drugs: These medications are crucial in preventing further bone damage caused by myeloma. They help alleviate bone pain and significantly reduce the risk of fractures, improving your quality of life.
Radiotherapy: For localized pain or specific areas of bone damage, radiotherapy can be an effective treatment to provide relief and improve mobility.
In cases where myeloma progresses slowly, your doctor may choose to monitor the disease closely before starting more aggressive treatments. For patients in good health, a stem cell transplant using their own blood stem cells (an autologous transplant) may be suggested. In fewer cases, a transplant from a donor (an allogeneic transplant) might be considered.
Learn more: Treatments for blood cancer and blood disorder
Outlook and managing Myeloma
The primary goal of treating myeloma is to control the disease and enhance your quality of life. The prognosis varies based on several factors, including the stage of myeloma at diagnosis, your age, overall health, the treatments applied, and how well the myeloma responds. Currently, about 50% of those diagnosed with myeloma live for more than five years, and around 30% live more than ten years after their diagnosis. It's important to remember that these statistics are based on monitored survival in clinical trials and do not define individual outcomes.
Advancements in research and ongoing clinical trials are consistently improving the understanding and treatment of myeloma. Regular monitoring by healthcare professionals is essential to manage the disease effectively and adapt treatments as necessary. By staying informed and proactive in managing myeloma, you and your healthcare team can significantly influence the effectiveness of your treatment and your overall well-being.
Learn more: Blood cancer research at DKMS
A blood cancer or a blood disorder diagnosis can feel overwhelming, but remember, you're not alone. Our team is here, ready to provide the support and guidance you need. Partnering with DKMS can help you share your story and amplify our combined efforts to expand the stem cell registry. This increases the chances of finding a potentially lifesaving match if a stem cell transplant becomes necessary.
Your well-being is our priority, and we're committed to walking alongside you every step of the way, so do reach out to us. Together, we can create more hope and opportunities for people living with blood cancer.
References
1. Multiple myeloma. BMJ Best Practice. Last reviewed February 2021.
2. What is myeloma? How does myeloma develop? Cancer Research UK. Last reviewed July 2023.
3. What is myeloma? What are plasma cells? Cancer Research UK. Last reviewed July 2024.
4. Multiple myeloma: Aetiology. BMJ Best Practice. Last reviewed February 2021.
5. Myeloma incidence statistics. Myeloma incidence by age. Cancer Research UK. Last reviewed June 2024.
8. Myeloma symptoms. Cancer Research UK. Last reviewed July 2024.
9. Myeloma survival. Cancer Research UK. Last reviewed July 2024.